Hunger Block™ Procedure
A New Solution When Weight Loss Medications Stop Working

A New Solution When Weight Loss Medications Stop Working
The Hunger Block™ Procedure—our name for a medical technique called bariatric embolization—offers long-lasting help for people whose weight loss has stalled on popular medications like Wegovy® or Ozempic®. If feeling hungry, struggling with cravings, or hitting a plateau has become a problem, this procedure could make a difference by working alongside your current medicine to tackle hunger from a new angle¹².
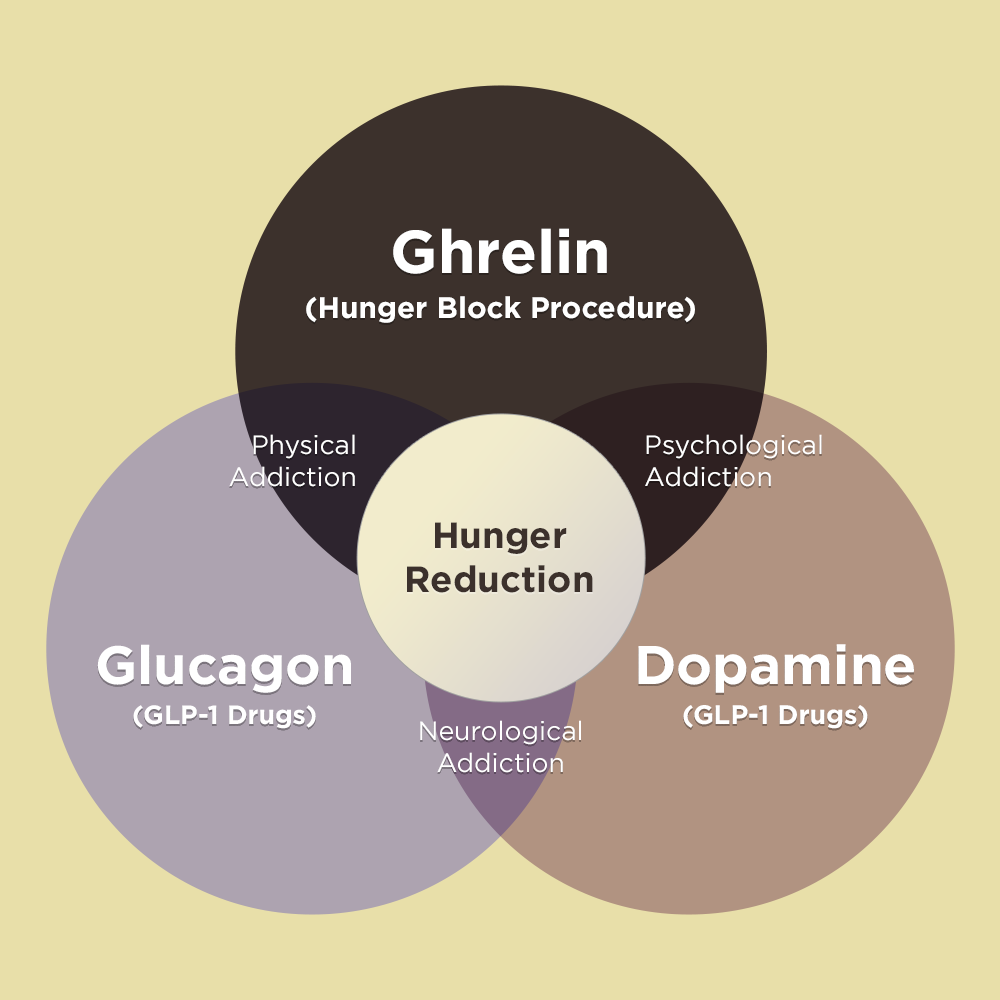
How Do GLP-1 Weight Loss Medications Work?
Medications like Ozempic®, Wegovy®, and Mounjaro® are known as GLP-1 receptor agonists. Here’s how they help with weight loss:
- They help your body control blood sugar
After you eat, these medications boost insulin (which lowers blood sugar) and lower glucagon (which stops blood sugar from spiking)²³. - They help you feel full sooner
GLP-1 drugs slow how quickly food leaves your stomach, so you feel fuller longer⁴. - They help reduce cravings
These medications send signals to areas of the brain involved in pleasure and reward, making highly tempting foods (like sugary snacks and fatty treats) less appealing for many people⁵.
Still, while you may eat less often and feel fuller, these medications may not stop all food cravings—especially for foods high in sugar or fat⁶⁷.
Has Your Weight Loss Stalled?
Why Isn’t Weight Loss Always Enough
Even while taking a GLP-1 medication and eating less, it’s possible to hit a weight loss plateau, especially if you still eat a lot of sugary or fatty foods:
- Some foods pack in a lot of calories
Even small amounts of candy, pastries, fried foods, or ice cream can add up quickly, making it hard to lose more weight⁶. - Habits and cravings can be strong
Your brain still enjoys and seeks out these tasty foods, which can overpower your body’s “fullness” signals⁷.
This is why some people lose less weight than expected with medication alone—and why helping tackle these cravings directly can make all the difference⁸.
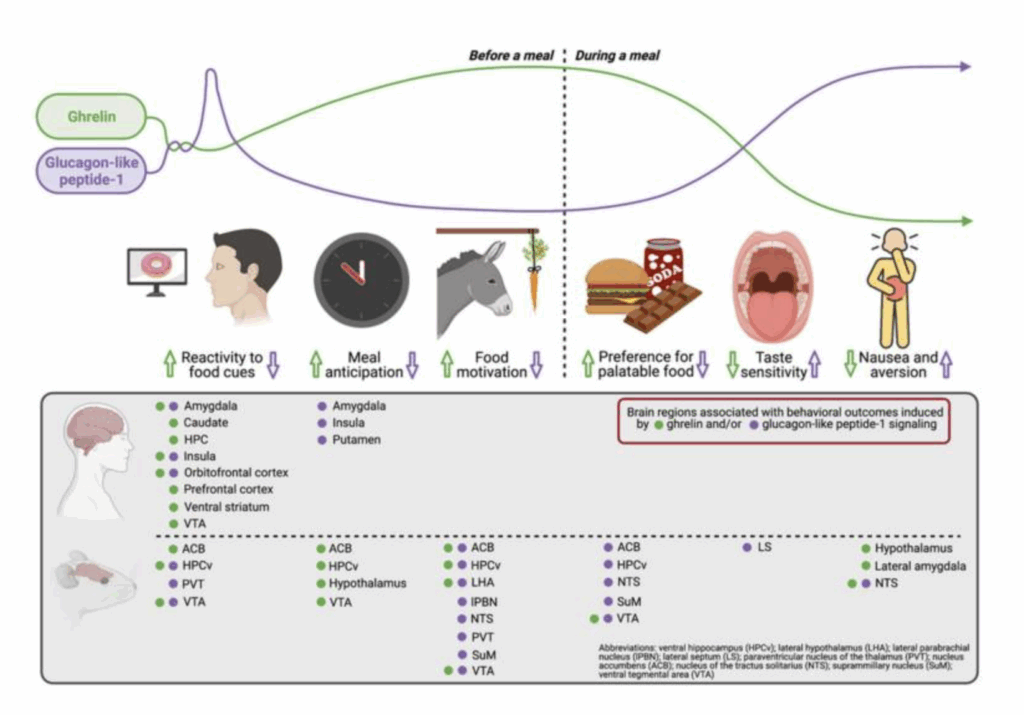
Ghrelin and GLP-1 work like “opposite signals” in the body when it comes to craving and enjoying tasty, high-fat or high-sugar foods. Ghrelin increases hunger, boosts food cravings, and makes food seem more appealing—especially before eating or when anticipating a favorite meal. GLP-1, on the other hand, reduces those cravings, lowers interest in indulgent foods, and can even make some foods less pleasant by affecting taste or causing mild stomach discomfort. Together, they influence how much effort you’re willing to make to get certain foods, how appealing those foods seem, and how your brain reacts to seeing or smelling them.
Before you eat, your body’s “hunger hormone” ghrelin ramps up food cravings, especially for sweets and high-fat foods, making them seem more rewarding and worth the effort to get. The hormone GLP-1 works in the opposite way—it calms cravings, reduces interest in rich foods, and may make them taste less appealing. Ghrelin pushes you toward wanting and seeking certain foods, while GLP-1 helps you slow down or avoid overeating. Balancing these two signals can be import in ant for weight control and healthy eating habits.
Why Choose Us
Break Through Weight-Loss Plateaus
The Hunger Block™ Procedure® helps when medications like Ozempic® or Wegovy® stop working by reducing hunger hormones for lasting appetite control.
A Minimally Invasive Way to Curb Cravings
Using advanced imaging, a specialist safely blocks the stomach’s hunger-producing artery, lowering ghrelin levels and easing cravings for sugary and fatty foods.
Better Results Through Dual Therapy
Combining GLP-1 medications with the Hunger Block™ Procedure balances hunger and fullness signals to achieve steady, long-term weight loss.
Popular Practices
How the Hunger Block™ Procedure Works
The Hunger Block™ Procedure is a minimally invasive treatment that lowers the body’s main hunger hormone, called ghrelin. Here’s what happens:
- A specialist places a very thin tube through an artery in your wrist or groin and “blocks” (embolizes) a blood vessel that supplies the upper part of your stomach, where most ghrelin is made⁹.
- With less blood flow, your stomach produces far less ghrelin. This means you feel fewer strong, stubborn hunger signals—especially the cravings for snacks or comfort foods¹⁰.
- The effect is long-lasting and can help people eat less, fast more easily, and avoid impulse snacking¹¹.
- Most people see hunger drop and weight decrease—on average, about 6% to 8% of their total body weight within several months¹².
Why Using Both Treatments Together Works Best
- Combining GLP-1 medications with the Hunger Block™ Procedure gives you two ways to control eating: The medication helps you feel full and makes it easier to say no to tempting foods⁵.
- The procedure reduces hunger at its source, especially stopping the intense desire to snack, binge, or eat out of habit¹⁰.
- This teamwork is especially helpful for breaking through plateaus—when weight loss slows or stops despite staying on your program¹².
What Happens to Hunger and Cravings After Dual Therapy?
The chart below shows how hunger hormone (ghrelin) and fullness hormone (GLP-1) levels change at different points in the day. When both treatments are used:
- Ghrelin is much lower, so hunger and cravings are milder—even during fasting or between meals.
- GLP-1 levels after meals stay high, which means you feel full, satisfied, and less tempted by junk food.
Average blood levels of ghrelin and GLP-1 throughout the day: baseline, GLP-1 medication, and GLP-1 + Hunger Block™ Procedure.
Our Latest Articles
Inside the Procedure: What Really Happens During Bariatric Embolization
A Precise Non-Surgical Approach to Weight Loss Bariatric embolization also known as the Hunger Block Procedure is performed by interventional…
When Weight Loss Medications Stop Working: Why the Hunger Block™ Procedure Complements GLP-1 Drugs
Why Weight Loss Medications Don t Always Work Forever GLP- medications like Ozempic Wegovy and Mounjaro have changed millions of…
From First-in-the-Nation to the Future: How Bariatric Embolization Is Changing Obesity Treatment
A Groundbreaking Step in the Fight Against Obesity In physicians at Dayton Interventional Radiology made history by performing the first…
References and Bibliography
Glucagon-Like Peptide-1 Receptor Agonists
Author: K. Huffman, L. Trujillo, C. Cuomo
Source: StatPearls (NCBI Bookshelf)
Date: February 28, 2024
The Effects of Dual GLP-1/GIP Receptor Agonism on Glucagon Secretion in Humans
Author: C.C. O’Neill, K. Kolterman
Source: Frontiers in Endocrinology
Date: August 21, 2019
Striking the Balance: GLP-1/Glucagon Co-Agonism as a Treatment Strategy for Obesity
Author: Richard R. Holst, et al.
Source: Frontiers in Endocrinology
Date: September 7, 2021
Your Friendly Guide to GLP-1 Weight Loss: What Works, What Doesn’t, and What’s Next
Author: Intermountain Healthcare, editorial staff
Source: Intermountain Healthcare, Blog
Date: March 18, 2025
Can GLP-1 Be a Target for Reward System Related Disorders? A Review of Preclinical and Clinical Evidence
Author: E. Ertugrul, S. Yazici
Source: Frontiers in Psychiatry
Date: January 17, 2021
Research Shows GLP-1 Drugs Are Effective But Complex
Author: UChicago Medicine Editorial Team
Source: University of Chicago Medicine
Date: May 29, 2024
Dietary Intake by Patients Taking GLP-1 and Dual GIP/GLP-1 Receptor Agonists
Author: C. Andersen, T. Müller, et al.
Source: Frontiers in Nutrition
Date: July 24, 2024
Bariatric Artery Embolization for Obese Patients. An Up-to-Date Review
Author: S. Jose, S. Jha, T. Oklu
Source: Journal of Clinical Medicine
Date: September 25, 2023
Bariatric Left Gastric Artery Embolization for the Treatment of Obesity
Author: T. Kim, J. Shin, T. Oklu
Source: American Journal of Roentgenology
Date: December 22, 2015
Ghrelin Stimulates Gastric Emptying and Hunger in Normal-Weight Humans
Author: G.H. Cummings, J. Overduin
Source: Journal of Clinical Endocrinology & Metabolism
Date: August 31, 2006
Ghrelin and Glucagon-Like Peptide-1: A Gut-Brain Axis Battle for Food Reward
Author: S. Kroemer, H. Small
Source: Frontiers in Endocrinology
Date: March 16, 2021
GLP-1 and the Neurobiology of Eating Control: Recent Advances
Author: N. Berthoud, A. Münzberg
Source: Endocrinology
Date: January 5, 2025
Bariatric Embolization: Are Patients Actually Losing Weight?
Author: J.A. Hause
Source: Endovascular Today
Date: April 12, 2018